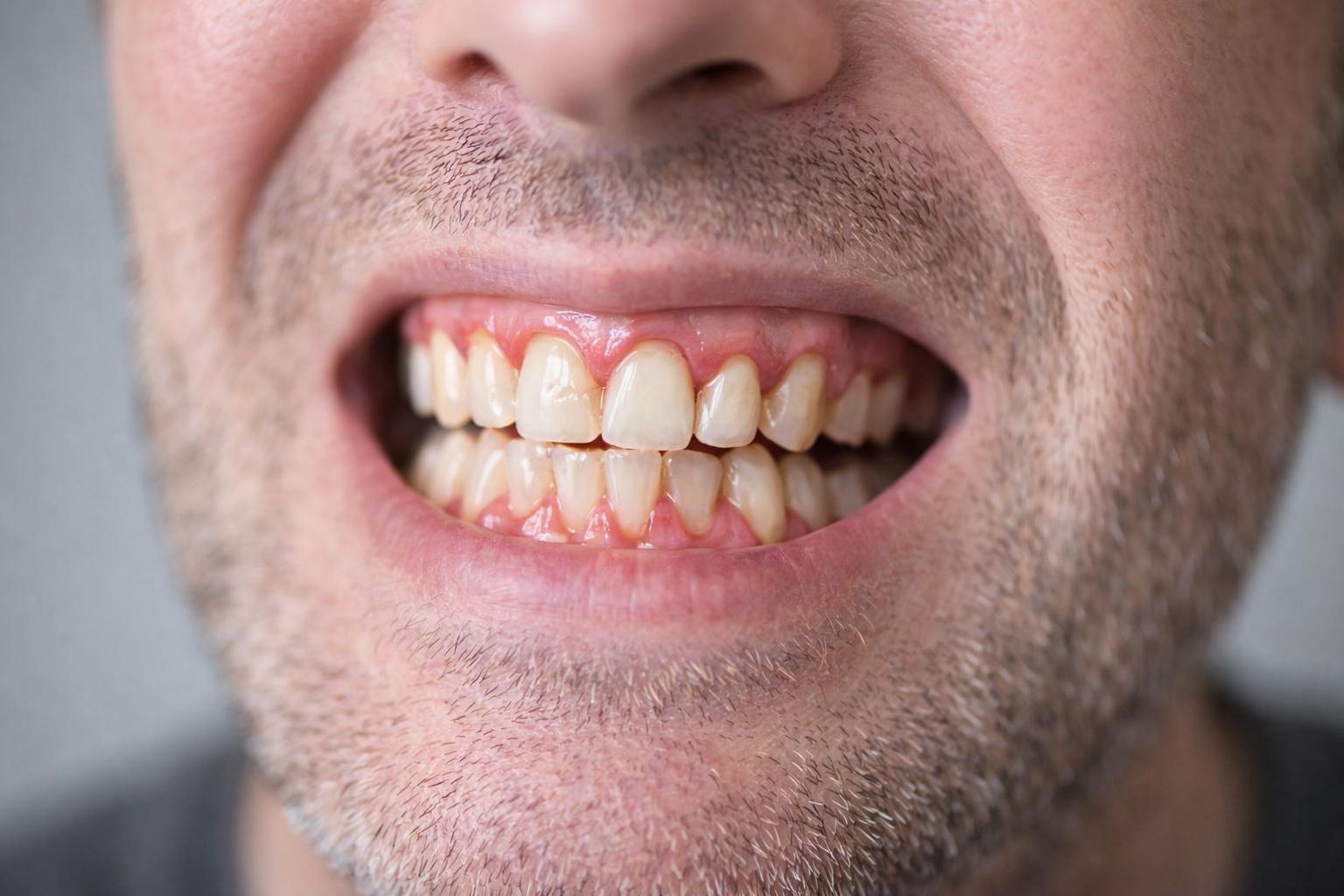
Receding Gums: What’s Really Causing Them — and What You Can Actually Do
Receding gums are often misunderstood.
Many people assume they’re a sign of poor brushing, or simply “getting older”. Others only notice when teeth start to look longer, or sensitivity creeps in and doesn’t quite go away.
In reality, gum recession is a biological response to stress and inflammation. And while some of the causes are fixable, others need careful management rather than quick solutions.
Understanding what’s actually happening is the first step in knowing what to do next
What gum recession actually is
Healthy gums sit snugly around the neck of each tooth, forming a protective seal.
When gums recede, that seal gradually moves downward (or upward, on upper teeth), exposing the root surface of the tooth. Unlike enamel, roots aren’t designed to be exposed. They’re more sensitive, more vulnerable to decay, and harder to keep clean.
Gum recession doesn’t usually happen suddenly. It develops slowly, often without pain, which is why it’s easy to miss in the early stages (so many of my patients are surprised when they realised they’ve not spotted it themselves at home, but as it’s so incremental, it can be really tough to notice).
Visual signs to watch for
People often notice recession before a dentist does, they just don’t always recognise it for what it is.
Common signs include:
Teeth appearing longer than they used to
A visible notch or step near the gumline
Yellowish areas at the base of the tooth (this is exposed root, not plaque)
Increased sensitivity to cold or touch
Gums that look thinner or uneven
Bleeding isn’t always present. In fact, recession can progress quietly even when gums don’t bleed at all.
The most common causes of receding gums
Gum disease
This is the most frequent cause.
Plaque buildup along the gum line triggers inflammation. Over time, that inflammation damages the supporting tissues, allowing the gums to pull away from the teeth. Left untreated, this process can also lead to bone loss.
Importantly, gum disease isn’t always painful (in fact, in the early stages, it very rarely is) which is why regular dental and hygiene checks matter.
Overzealous brushing
Brushing harder does not mean brushing better.
Using excessive pressure, especially with a manual toothbrush or a firm-bristled brush, can wear away gum tissue over time. This type of recession often appears as sharp, clean notches near the gumline.
People who are very diligent about oral hygiene are sometimes the most surprised by this.
Tooth position and bite
Teeth that are crowded, rotated, or sit outside the main arch may have thinner gum coverage. These areas are more prone to recession, even with good cleaning.
Grinding or clenching can also place excess forces on certain teeth, contributing to gum movement over time.
Genetics and anatomy
Some people naturally have thinner gum tissue. This doesn’t mean recession is inevitable, but it does mean the margin for error is smaller.
Hormonal changes, smoking, and previous orthodontic treatment can also play a role.
Manual vs electric toothbrushes — does it matter?
It can.
Electric toothbrushes, particularly those with pressure sensors, tend to reduce the risk of overbrushing. They do the work for you, meaning less scrubbing is needed.
Manual brushes aren’t inherently bad, but technique matters more. Soft bristles, gentle pressure, and brushing along the gumline rather than across it are key. We actually have a Toothbrushing Coach Tool on the site (it’s free), which can give you an indication of how your brushing style might be affecting your tooth anatomy.
If you’re looking to do a bit more of a deep dive into whether electric toothbrushes out-perform their manual counterparts, take a look at our recent reviews of exactly what kind of electric toothbrushes are out on the the market at the time of reading.
Can receding gums grow back?
This is where expectations matter.
Lost gum tissue does not naturally regenerate. Once recession has occurred, the goal is usually to stop it progressing, not to reverse it.
That said, many cases can be stabilised with:
improved brushing technique
better plaque control
regular hygiene appointments
addressing bite or grinding issues
When the underlying cause is managed early, recession can remain unchanged for years.
When surgery becomes part of the conversation
Gum grafting or periodontal surgery is usually considered when:
recession is progressing despite good care
roots are severely exposed
sensitivity is affecting daily life
aesthetics are a significant concern
there’s a risk of further bone loss
The main goal is preserving what remains and preventing long-term damage and deteriorating quality of life as a result of gum recession (which can lead to tooth and bone loss without care and treatment).
A periodontist (a gum specialist) can assess whether surgery is appropriate, or whether monitoring is the safer option. If you’re anxious about surgery, there are many dentists who now offer intravenous (IV) sedation to help you relax. It’s a really groundbreaking technique for surgical procedures, though many people also have it for more routine procedures like a root canal.
How to keep an eye on it
Gum recession is best managed early.
That means:
regular dental check-ups
routine hygiene visits
asking specifically about gum levels, not just cavities
monitoring changes in sensitivity or appearance
Photos taken at home can also help track subtle changes over time.
The bigger picture
Receding gums aren’t a personal failure, and they’re not something to ignore. They’re a signal, and one that deserves calm, informed attention rather than panic or aggressive self-fixing.
If you understand what’s happening, you’re already in a much better position to protect your smile long-term. We at Nova can help put you in a more knowledgable position about your gum health.
Contact us for free guidance, and feel more in control over the destiny of your dental health.